Author: Benita Willis | February 7, 2018
Article by Brad Beer from Physic With A Finish Line.
The psychological impact of injury and pain
I routinely advise clients that as a physiotherapist I do not despite popular opinion treat people’s pain. Rather I treat the psychological unrest that the pain or injury is creating for the individual. I often say that people are ‘tough’. They can actually put up with physical and mechanical pain. Quite often they can tolerate pain, and even worsening pain for significant periods of time. In many cases it is only when the physical pain begins to limit people in doing the physical things that they love to do that emotions such as fear, anxiety, and frustration can build.
I personally have experienced frustration, anxiety, and fear driven by injury and physical restrictions brought about by injury and physical pain over my many years of being physically active.
Patellofemoral pain
Patellofemoral pain affects physically active and sedentary individuals, and accounts for 11–17% of knee pain presentations to general practice (1) and 25–40% of all knee problems seen in a sports injury clinic (1). It is also one of the most costly forms of knee pain, having a 23% prevalence in the UK population (2).
Patellofemoral pain is characterised by anterior knee pain associated with activities that load the joint (see image below) such as squatting, rising from sitting, climbing stairs, and running.
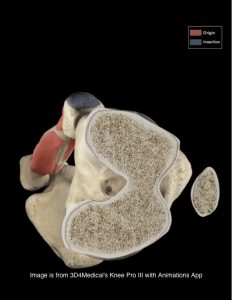
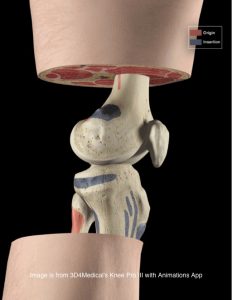
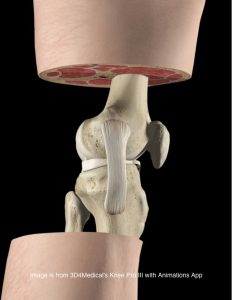
Symptoms may include pain behind the kneecap (retropatellar pain), or around the kneecap (peri-patellar pain). The pain may be dull in nature or at time also sharp in nature when loaded such as with a single leg decline squat test.
PFP has traditionally been viewed as self-limiting and ‘benign’. However emerging literature is highlighting that for many sufferers pain can persist for many years, resulting in a decline in sports participation. Indeed it appears that for many sufferers of PFP the long term prognosis is relatively poor (3).
A 2012 paper (3) that looked at 310 sufferers of PFP found that only ? of patients are pain free 1 year after their diagnosis of PFP, and 91% still reported pain and dysfunction four years post diagnosis. Such patients invariably end up withdrawing from sports participation and physical activities, and may develop fear avoidant behaviors and catastrophizing thoughts about their knee pain.
The biopsychosocial model of pain
Psychological distress has been identified in lower back pain and tendon sufferers through systematic reviews (2), however never before in PFP patients.
The biopsychosocial model of persistent pain has recognised that factors such as fear avoidant behaviours and catastrophising thoughts can modulate physiological responses to pain, by way of the development and persistence of pain.
Current models of persistent pain have identified the importance of thinking biomechanically (ie beyond muscles and joints). Appropriate studies may provide an insight that may lead to development of ideas about the biopsychosocial model of pain.
My own experience with patellofemoral pain
My greatest challenges being dealing with the frustration, and a depressed state around patellofemoral pain with my knees. My left knee 12 years ago, and my right knee just recently (as I write this I am four months post surgery).
A focus on the ‘experience’ of living with patellofemoral pain
When I came across a paper published while scrolling my Twitter feed that was looking at the experience of living with patellofemoral pain I was personally very interested, and professionally eager to read the article.
The purpose of the paper (1) was to investigate the experience of living with patellofemoral pain (PFP).
For many years the literature base for patellofemoral pain has been focussed on looking at the efficacy of treatments (eg exercise therapy, orthotic prescription etc), and also the analysis of contributory factors for the onset of patellofemoral pain, namely biomechanical in nature.
Hence it was refreshing to read a paper that was looking at the overall impact of ‘living with patellofemoral pain’ including the emotions of loss, confusion, and fear-avoidance behaviours. In my own journey in trying to find solutions for my patellofemoral joint pain I have experienced all of these.
What did the paper reveal?
The paper invited 10 participants (aged between 18 and 40 years) to give detailed reports of the impact that living with PFP had on their lives. This included:
- Loss of physical and functional ability
- Loss of self-identity
- Pain related confusion and difficulty making sense of their pain
- Pain-related fear
- Fear avoidance and ‘damage’ beliefs
- Inappropriate coping strategies
- Fear of the future
The Findings
Five major themes emerged from the data, as follows:
1. Impact on self:
Participants offered detailed accounts of the impact of PFP on their lives. Loss of self and loss of self-identity were reported by many of the study participants. PFP symptoms affected all of the study participant’s daily life. The pain was reported to be a pervasive and disruptive feature of the day that resulted in loss of physical ability. Loss of activities included: walking, driving, holidays, exercise, time with family and friend, playing with children, work duties, and kneeling. These loss of activities directly impacted the participant’s role and position within their social network, triggering feelings of loss and self-identity, including questioning their career aspirations.
It is known that loss of significant relationships is a key aspect of loss for people suffering from persistent pain, and participants in the study mirrored this finding by reporting that important and meaningful relationships has been disrupted.
2. Uncertainty, confusion and sense making
All participants expressed a strong desire to ‘sense make’ or understand the cause of their pain. The chief focus of the participant’s beliefs was that biomechanical factors were causative of their pain. Confusion was reported re the ‘flare up ‘ nature of PFP. Some participants recalled biomechanical diagnoses that had been given to them many years in the past, highlighting the influence and importance of words used and explanations given when consulting patients. Many participants expressed distress and confusion regarding their joint noises that accompanied their pain.
Many participants expressed a strong desire to pursue imaging (scans), and feeling like the health practitioner had not taken them seriously enough or been through enough if imaging requests were not organised.
Cultural beliefs around pain also influenced the participant’s sense making of their pain.
3. Exercise and activity beliefs
All participants reported specific beliefs regarding barriers to exercise and activity. Feeding into these beliefs was diagnosis uncertainty. Some participants held the belief that pain was a direct sign of ongoing tissue damage. Fear-avoidant behaviour patterns were commonly reported by the study participants, whereby they would avoid activities through fear of pain resulting and associated damage.
4. Behavioural coping strategies
A key coping strategy for participants was rest and avoidance of aggravating activities. Many believed that time was necessary for the healing process, and that aggravating activities should be avoided.
Using analgesia (pain medications) was a commonly reported coping strategy, as was using knee supports as a self-management strategy.
5. Expectations of the future
The majority of the participants expressed negative views about the future. They all expressed a desire to be pain free ahead of any aspirations for functional improvements, or improvements in their desired activities.
90% of participants held negative beliefs about the future and their long term prognosis. This was largely borne out of the sense that patellofemoral sufferers had very little control of their pain. Many of the participants had attended previously failed physiotherapy treatments.
The take home
Patellofemoral pain can have significant psychological effects on sufferers.
If you read this blog and resonate with the impact that PFP can have on your life and psychological well-being then I implore you to seek appropriate assistance by way of a physiotherapist who has a special interest in the management and treatment of patellofemoral pain. If you have any questions re the management of your own patellofemoral pain than please leave them in the below comments or email me confidentially b.beer@pogophysio.com.au.
Please note: I am available for SKYPE consultations for interstate, or overseas clients. To organise a consultation please email helpme@pogophysio.com.au and the POGO Physio team will be in touch.
Tips of how to reduce symptoms of PFP
The below list is by no means comprehensive but rather some easy to implement and be aware of strategies that may help you reduce your patellofemoral symptoms:
- Avoid excessive stair climbing (going down stairs typically worse and more provocative)
- Avoid impact loading activities such as jumping.
- Reduce exercise loads such as running. You may simply start by reducing your running volume by half.
- Speak to your health care team about appropriate medication to assist with pain management.
- Consult with a physiotherapist who has a special interest in the treatment and rehabilitation of patellofemoral pain.
Physio With a Finish Line™,

Brad Beer (APAM)
Physiotherapist (APAM)
Author ‘You CAN Run Pain Free!’
Founder POGO Physio
Host The Physical Performance Show






